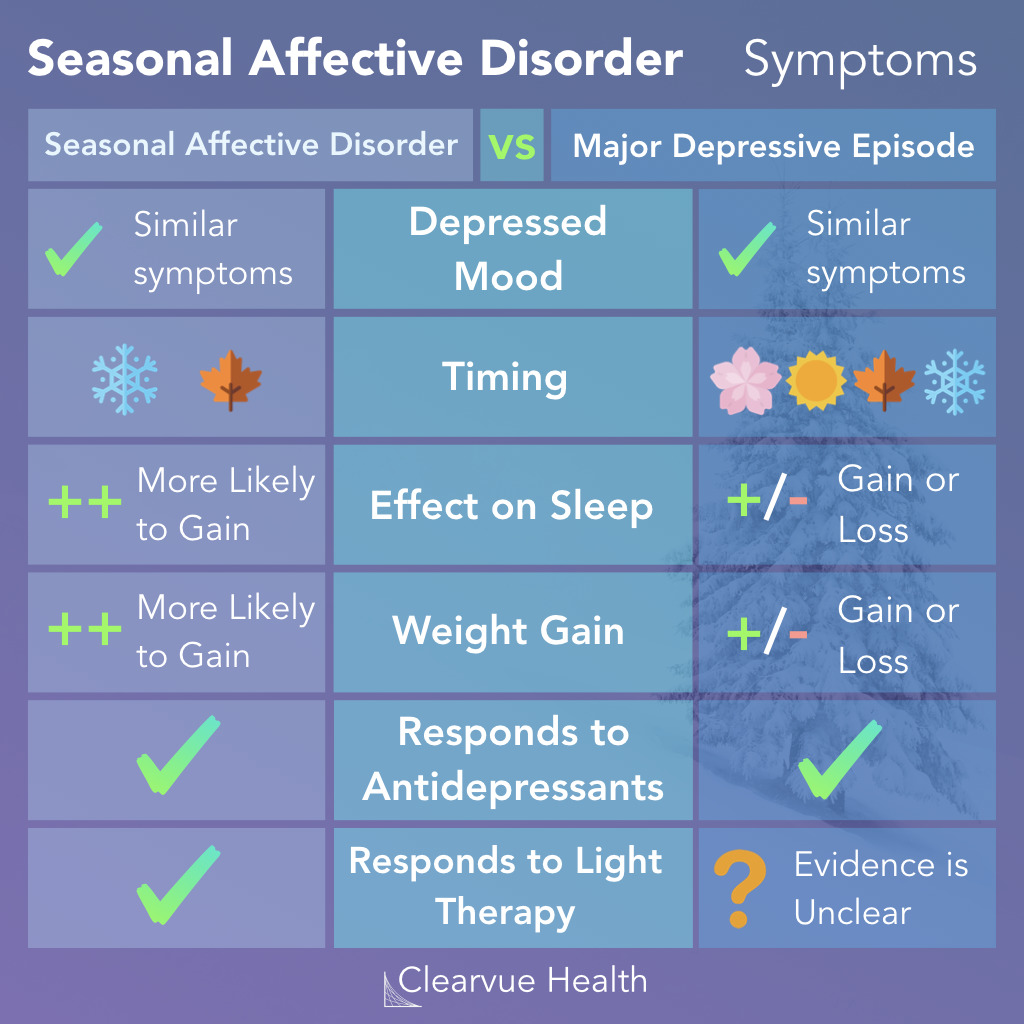
Seasonal Affective Disorder most often takes the form of a "winter depression." By definition, the diagnostic criteria of seasonal affective disorder are the same as that of depression.
However, seasonal affective disorder, as evidenced by the name, comes primarily during the winter and fall. Summer seasonal affective disorder also exists, but it is far less common.
Other than seasonality, the most notable differences between seasonal affective disorder and depressive disorders are the effects on sleeping and eating habits. Major Depressive Disorder can include both too little sleep (insomnia) or too much sleep (hypersomnia) while Seasonal Affective Disorder most often causes patients to need too much sleep.
Similarly, while Major Depressive Disorder can lead to both weight gain or weight loss, Seasonal Affective Disorder has most often been associated with weight gain, particularly a craving for carbs.
The Seasonal Patterns of Seasonal Affective Disorder
In order to quantify the "seasonality" of Seasonal Affective Disorder, researchers at the NIH asked patients to mark down which months they felt the best and which months they felt the worst.
Not surprisingly, everyone felt a little worse in the winter months, which is completely normal. Few patients felt that January was their best month or that July was their worst month.
Patients with Seasonal Affective Disorder showed the most striking pattern, reporting feeling happiest in June and July, while feeling the worst from December to February.
How Common is Seasonal Affective Disorder?
Many studies and researchers have different definitions of Seasonal Affective Disorder, leading to different estimates of the prevalence of Seasonal Affective Disorder. The largest studies have estimated that around 2-3% of people have it in North America.
In order to look at the relationship between Seasonal Affective Disorder and other psychiatric conditions, we used data from the NESDA, a large depression study of 2185 patients in the Netherlands.
We included both patients who met the stringent diagnostic criteria for depression as well as patients who had substantial symptoms but did not fully meet the full DSM depression criteria.

In the above data, we can see that patients who have had at least one diagnosis of either anxiety or depression have a much higher chance of getting Seasonal Affective Disorder.
Having a history of both anxiety and depression increases your risk more than 5x.
Bipolar patients have the highest risk of seasonal affective disorder, which is expected given that bipolar disorder by definition includes symptoms that come and go with time.