Opioid overdose and follow up treatment: the likelihood of continued care by insurance status
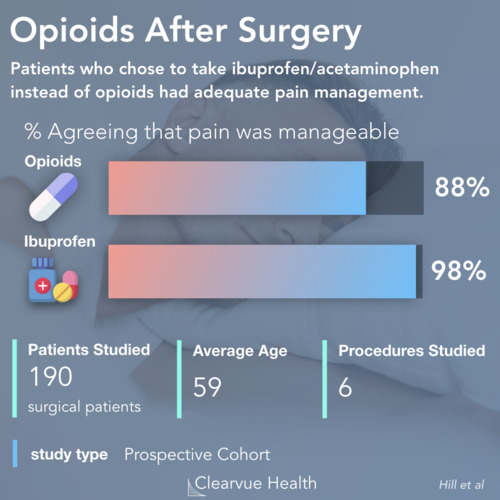
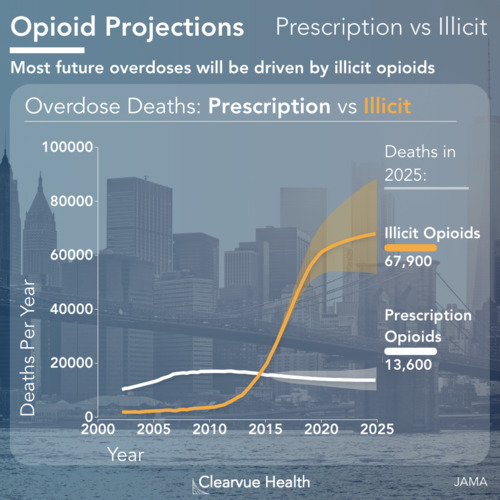
The opioid epidemic has been damaging the United States long before we even recognized it. All over the country, health professionals are recording unprecedentedly high rates of opioid use disorder. For someone who overdoses, fast treatment is required to save their life. The period after an overdose is a critical time for someone with opioid use disorder to be treated with medications and therapies. Unfortunately, the data is telling us that those in need of these treatments are not accessing them .
Data from insurance claims
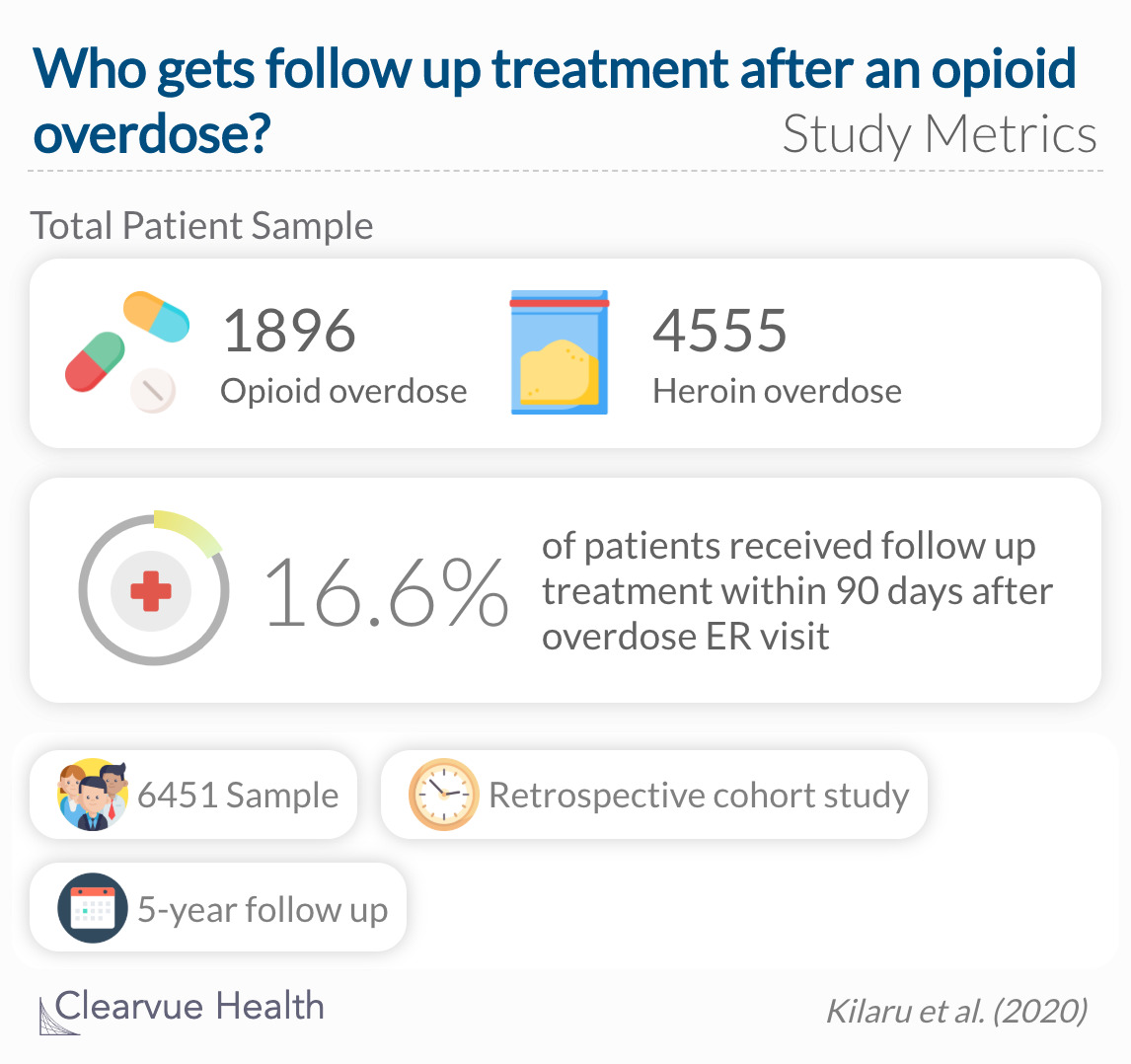
To understand the utilization of opioid use disorder services after an overdose, researchers collected 5 years of data from a large US commercial insurer. They identified every patient discharged from an emergency department after an opioid overdose. By the end of their search, they had national commercial insurance claims for 6451 patients. They analyzed whether or not any of these patients returned for follow up treatment within 90 days after their overdose.
For all patients in the study cohort, 1069 individuals (16.6%; 95% CI, 15.7%-17.5%) obtained follow-up treatment in the 90 days following overdose.
Source: Incidence of Treatment for Opioid Use Disorder Following Nonfatal Overdose in Commercially Insured Patients
The insurance records showed that only 16.6% of overdose patients received follow up treatment within the recommended 90 days after their emergency department visit. For these patients, it is not a lack of medical insurance that stopped them from getting follow up treatment. Other common reasons for not seeking treatment include a lack of affordability, concerns about stigma or a negative effect on job, and not being ready to stop using the substance.
Overdose type
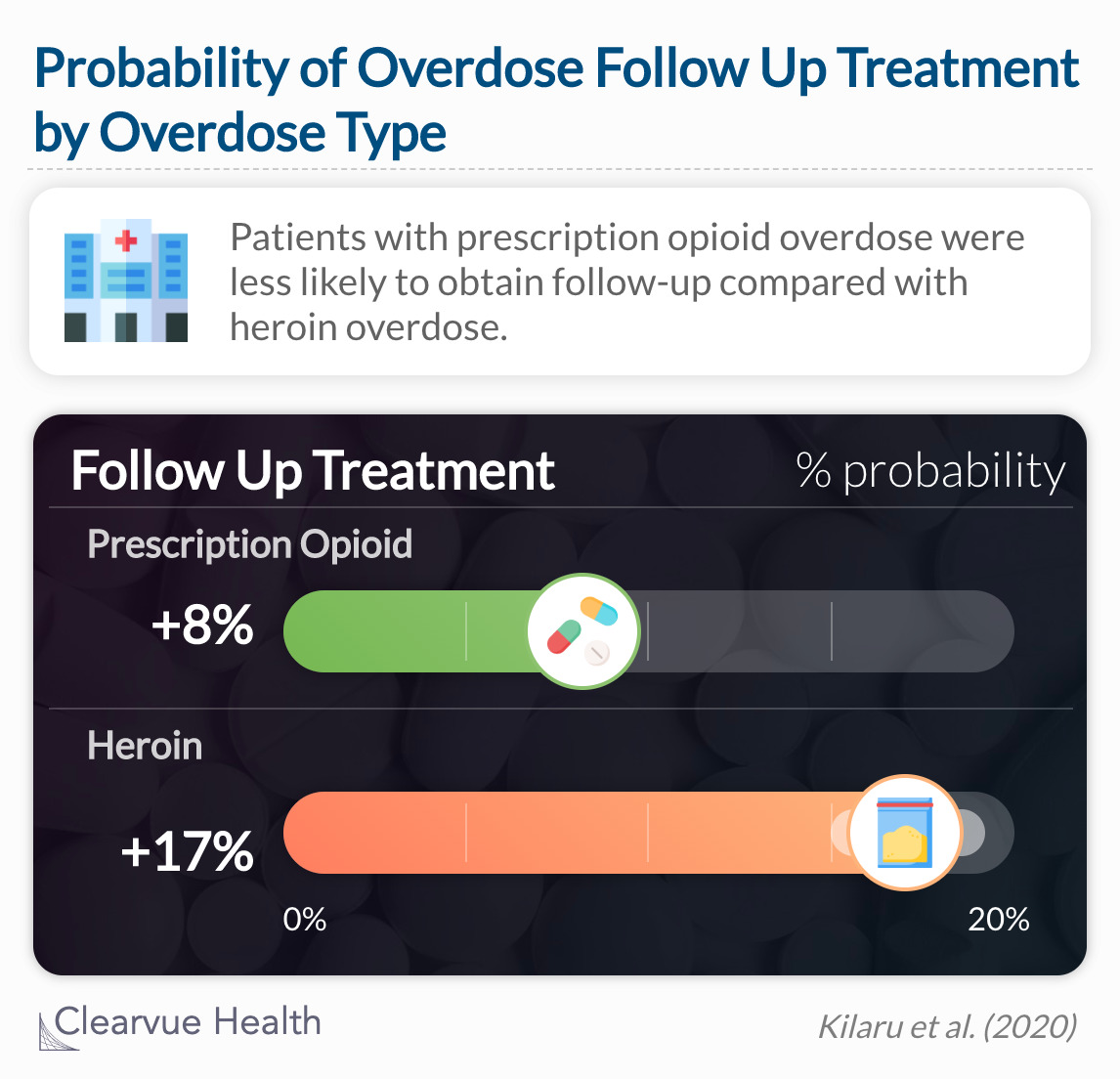
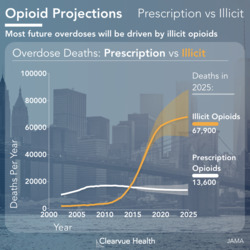
In the adjusted analysis for patients who did not receive treatment before the overdose, patients with prescription opioid overdose were less likely to obtain follow-up compared with a heroin overdose.
Patients with prescription opioid overdose were less likely to obtain follow-up treatment compared with a heroin overdose. Patients with heroin overdose significantly differed across all patient characteristics compared with those with prescription opioid overdose. They were younger, more likely to be male, and less likely to have received any medical treatment prior to their overdose. These traits may individually lessen a person's probability of follow up treatment.
Race
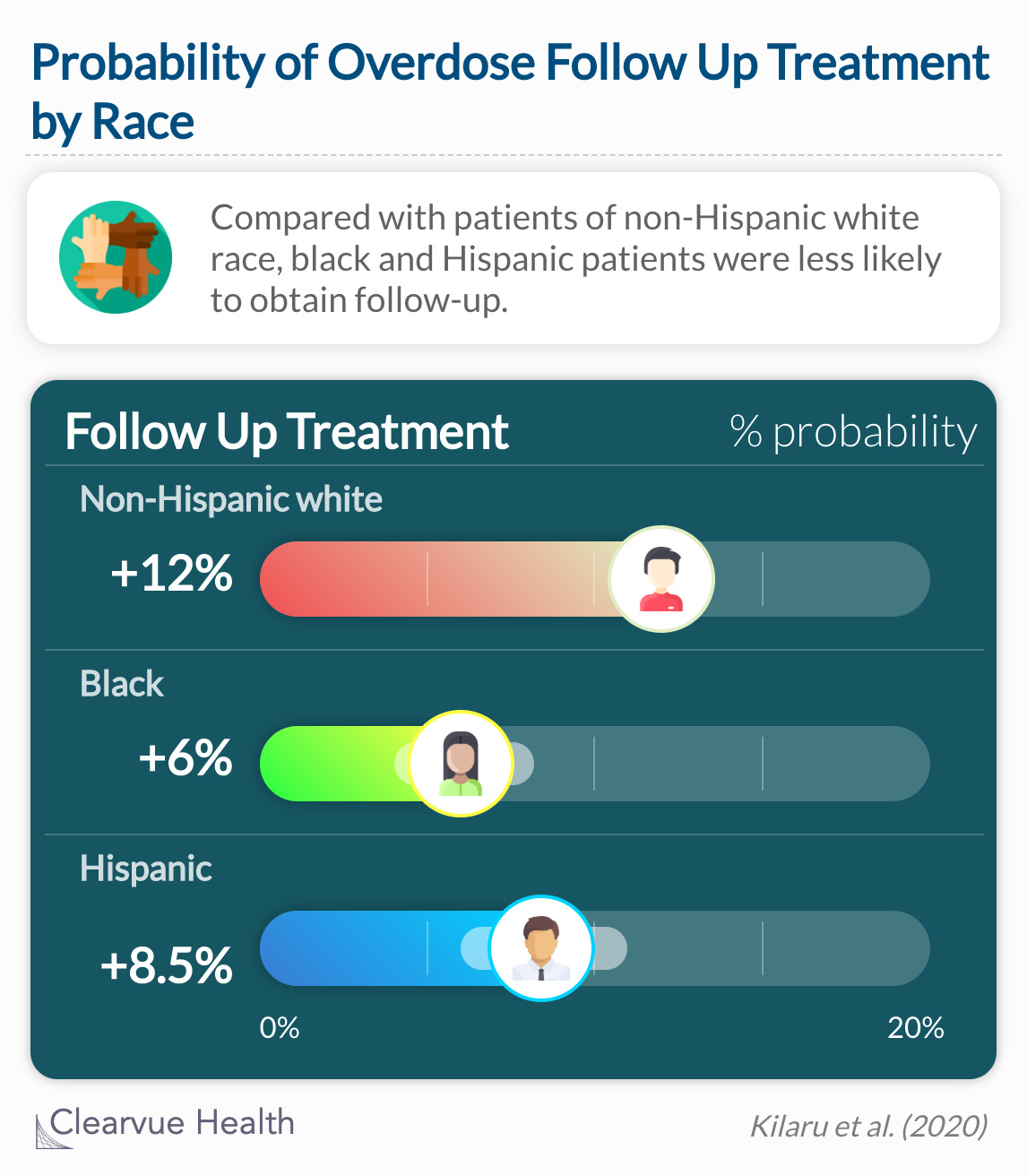
Compared with patients of the non-Hispanic white race, black (ARD, −5.9%; 95% CI, −8.6% to −3.6%) and Hispanic (ARD, −3.5%; 95% CI, −6.1% to −0.9%) patients were less likely to obtain follow-up.
Compared with non-Hispanic white patients, black and Hispanic patients were less likely to obtain follow-up. This disparity was present in both heroin and prescription opioid overdoses. Again, a lack of insurance can not be the reason for not receiving follow up treatment. It is possible that patient preferences, barriers to access, bias, or other causes can help explain this disparity.
Past anxiety treatment
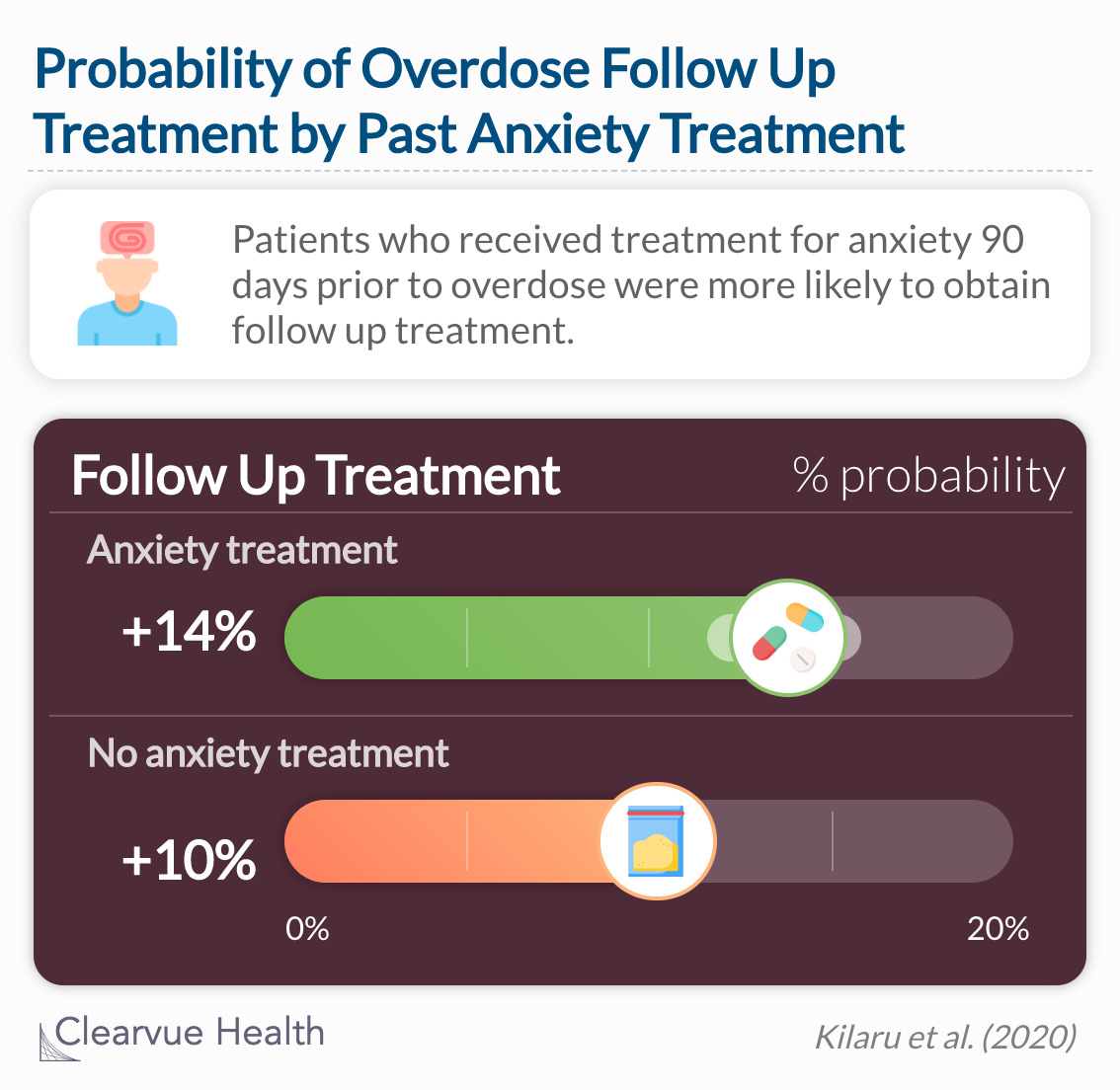
Patients with recent treatment for anxiety, including a treatment encounter for anxiety (ARD, 3.4%, 95% CI, 1.1%-5.8%) were more likely to obtain follow-up.
Interestingly, patients with recent treatment for anxiety, including a treatment encounter for anxiety, were more likely to obtain follow-up. Someone who has experience with health professionals may feel more comfortable seeking further medical attention than those who have little to no contact with health professionals. They may also hold more knowledge about the healthcare system as a whole and have an existing contact who could help lead them to the correct treatment.
The whole picture
“
Given that patients with commercial insurance likely have a superior ability to access care compared with patients who have public insurance, this persistently low rate suggests an opportunity for improvement.
JAMA
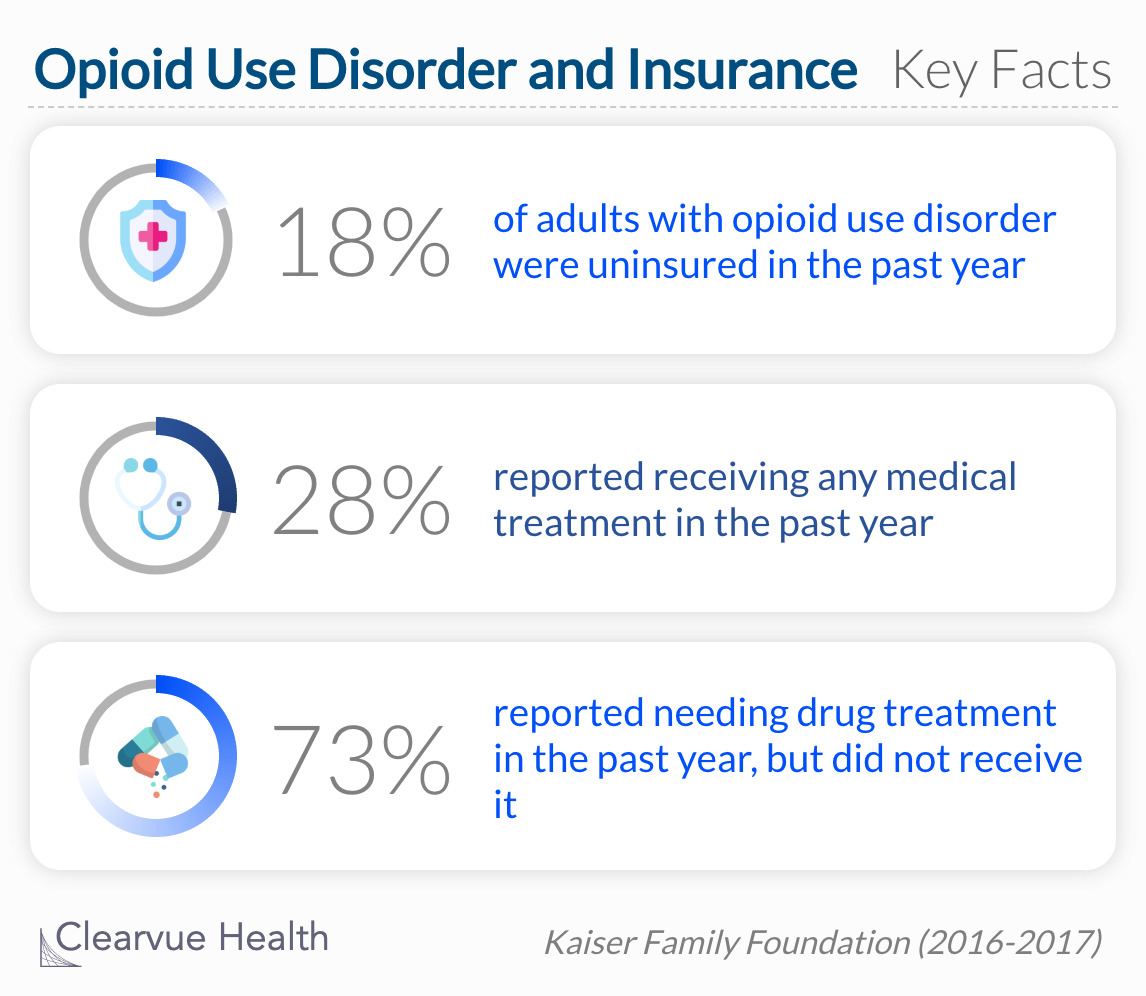
The study shows striking disparities in access to treatment and follow-up care. Even further, the study only includes participants with insurance and therefore does not encompass the entire population. Last year, the Kaiser Family Foundation released a report estimating that approximately 18% of those with opioid use disorders are uninsured. Those who are uninsured would not have been captured by the study above.
“
As the #opioidepidemic continues, nearly 1 in 5 of the 2 million nonelderly adults who have opioid use disorders are uninsured. Evidence indicates that individuals without health coverage are less likely to obtain needed treatments.
Kaiser Family Foundation
Nearly one-fifth (18%) of nonelderly adults with opioid use disorder were uninsured between 2016 and 2017.
In recent years, the rate of uninsured US citizens has hovered around 10%. In comparison, adults with an opioid use disorder have an uninsured rate of 18%, which is almost twice as high as the national average. Of uninsured opioid use disorder patients, many do not see a doctor yearly or when needed. With these facts, it is safe to assume that the proportion of people no receiving overdose follow up treatment is much higher when adding the uninsured population.