Ketamine has been used by many people over several decades. However, it has not been approved for human use in the United States. New research has shown that ketamine may actually be an effective antidepressant.
A new formulation that you spray into your nose has been shown to be effective in treating depression in several clinical trials. Based on this data, a key panel at the FDA has recommended its approval for treatment resistant depression.
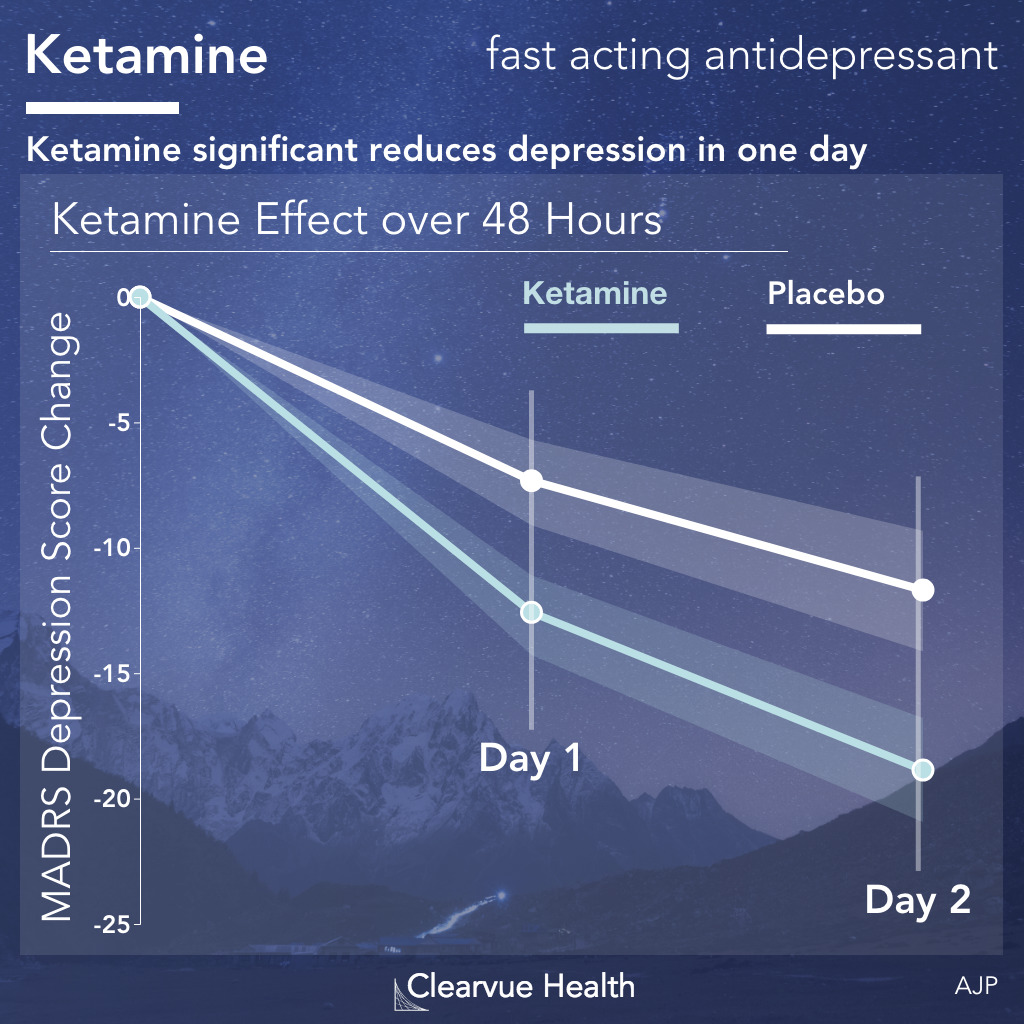
In one of the first clinical trials that drew wide-spread attention from medical professionals, researchers found that ketamine significantly reduced depression symptoms as soon as 24 hours after administration.
Source: Efficacy and Safety of Intranasal Esketamine for the Rapid Reduction of Symptoms of Depression and Suicidality in Patients at Imminent Risk for Suicide: Results of a Double-Blind, Randomized, Placebo-Controlled Study.
SSRIs, the mainstay of depression treatment today, can take weeks or months to take effect.
Source: Selective serotonin reuptake inhibitors (SSRIs)
Phase III Clinical Trial Data for Ketamine
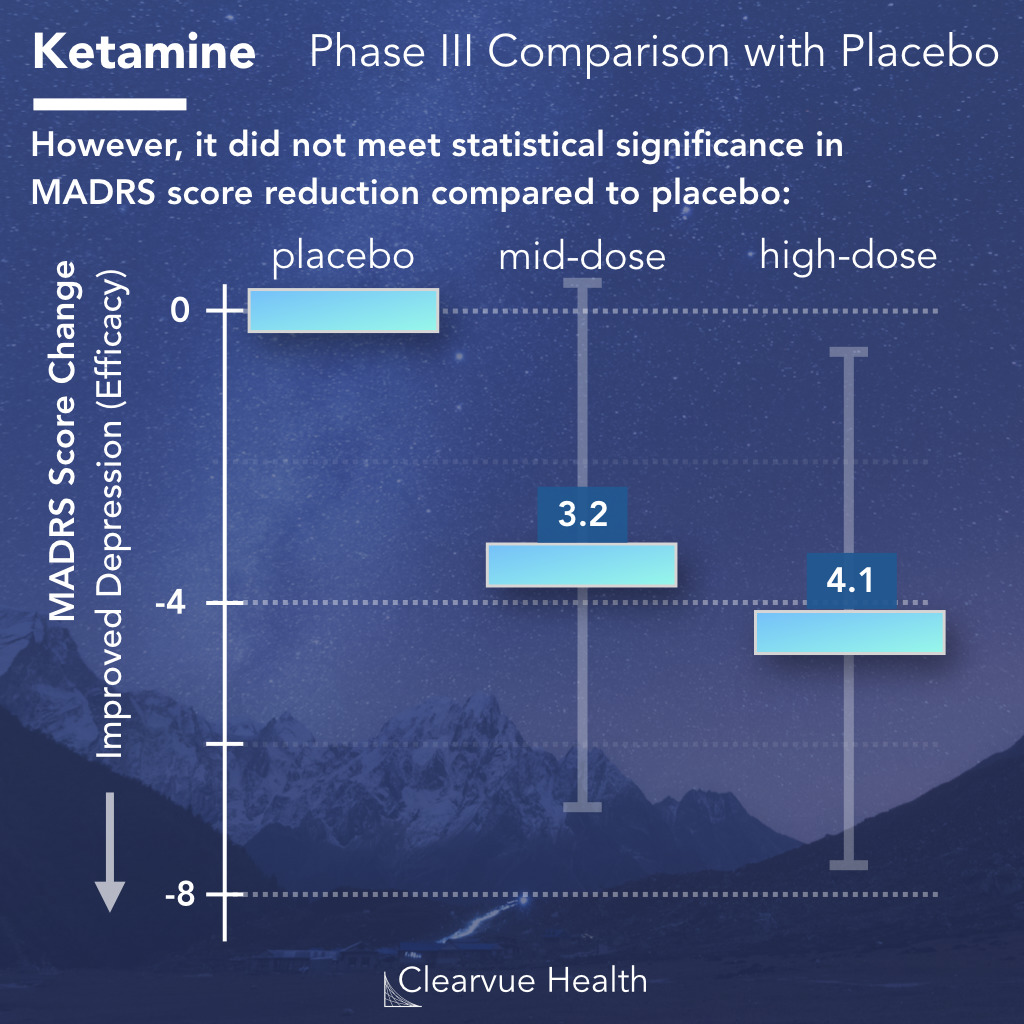
The Phase III data for ketamine showed some evidence of effectiveness, but overall it was mixed.
In order to get FDA approval, drug companies have to undertake multiple clinical trials. Phase III trials, the largest trials, usually produce the data used by the FDA to evaluate the effectiveness of a drug.
In one key phase III clinical trial, researchers evaluated two different doses of ketamine against a placebo control. All patients took an oral antidepressant as well.
After 28 days, doctors examined whether patients who took ketamine had an improvement in their depression compared to patients who only took the control.
They found that while on average, patients did better on ketamine, the results did not reach statistical significance, as shown by the gray error bars above.
Source: Janssen Announces Results of Esketamine Nasal Spray Phase 3 Study in Patients with Treatment-Resistant Depression
Ketamine + Antidepressant may increase response rates

The Phase III trial above also showed that ketamine may potentially increase response rates when combined with an oral antidepressant.
Patients who took ketamine along with an antidepressant were on average more likely to respond to treatment than patients who only took an antidepressant.
Over 28 days, more than half of patients who took high dose ketamine or mid dose ketamine showed significant declines in their depression symptoms. Patients who only took an oral antidepressant (Such as Zoloft or Prozac) only showed a 39% response rate.
Low Response Rates in SSRIs

If the phase III response rate data is confirmed in future trials, this would be an enormous gain for depressed patients.
SSRIs, the most popular antidepressants today, are the best depression treatments ever developed. However, they only work for some patients. Both Zoloft and Prozac have response rates less than 50%.