How Lyme Disease Causes Arthritis
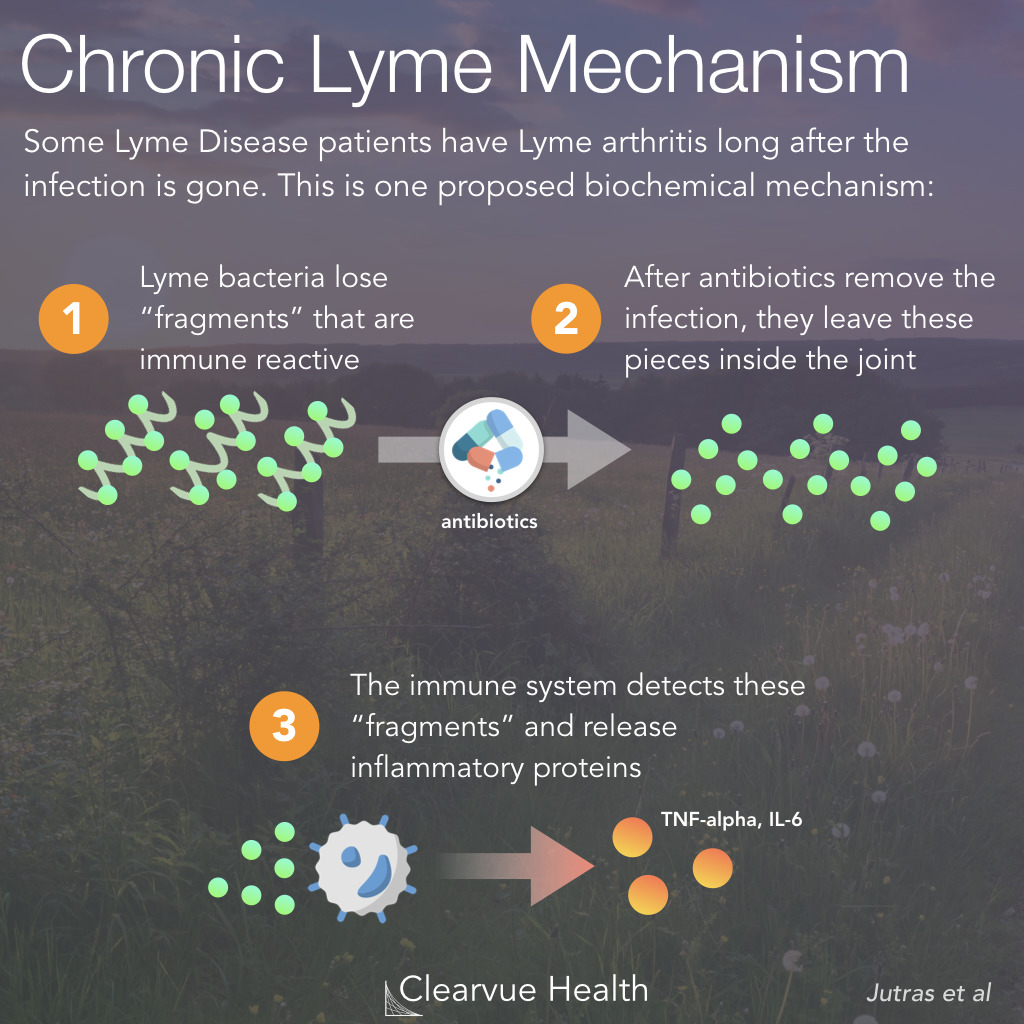
Figure 1: Chronic Lyme Disease Mechanism. Some Lyme Disease patients have Lyme arthritis long after the infection is gone. This is one proposed biochemical mechanism. Lyme bacteria lose “fragments” that are immune reactive. After antibiotics remove the infection, they leave these pieces inside the joint. The immune system detects these “fragments” and releases inflammatory proteins.
Chronic Lyme disease is one of the most controversial topics in medicine. Thousands of patients swear that they have it, yet many doctors and infectious disease specialists do not believe that it exists because of a lack of molecular evidence, among other reasons.
A new study in one of the most prestigious journals in science provides compelling evidence that there actually may be a biological mechanism behind chronic Lyme arthritis.
Their experiments suggest that the bacteria behind Lyme Disease contain a compound that is difficult to detect. Even after the bacteria are killed with an antibiotic, this compound can remain inside joints.
The immune system can recognize this compound and cause inflammation in the joint.
How is Lyme Disease Transmitted?
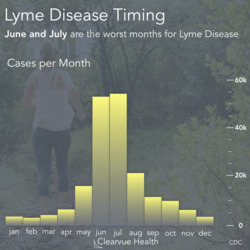
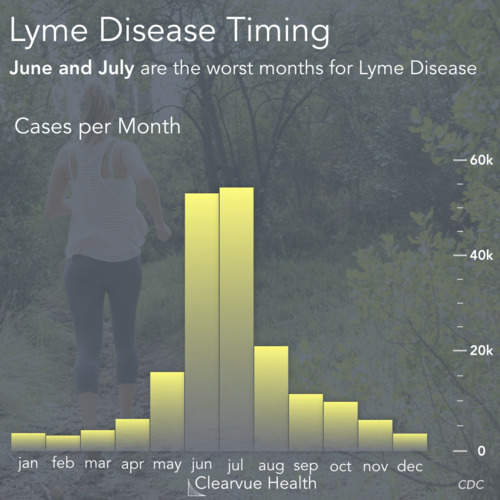
Lyme Disease comes from ticks. Ticks carry Lyme Disease and they can transmit it humans. Typically, these ticks stand on tall grasses, bushes, and wooded trails and wait to come in contact with a passing human or dog. They can then attach themselves onto the skin and begin to feed on blood. This is not painful and often goes undetected, which is why Lyme Disease can be so difficult to catch. It takes around 36 to 48 hours for a tick to transmit Lyme Disease.
Source: Borrelia burgdorferi peptidoglycan is a persistent antigen in patients with Lyme arthritis
Experimental Evidence for Chronic Lyme

Figure 2: Experimental Evidence for Chronic Lyme. Researchers found that human immune cells signal for inflammation when they added Lyme peptidoglycan, the proposed cause of Chronic Lyme. They found that white blood cells released many more inflammatory proteins, otherwise known as cytokines, after exposure to Lyme peptidoglycan (yellow-red) when compared to cells that were not exposed (blue-green).
In a lab experiment, researchers found that exposing human immune cells to this compound caused immune cells to start signaling for an inflammatory response.
Within the body, this type of response would cause redness, swelling, and pain.
Lyme Peptidoglycan is only present in joints of Lyme arthritis patients
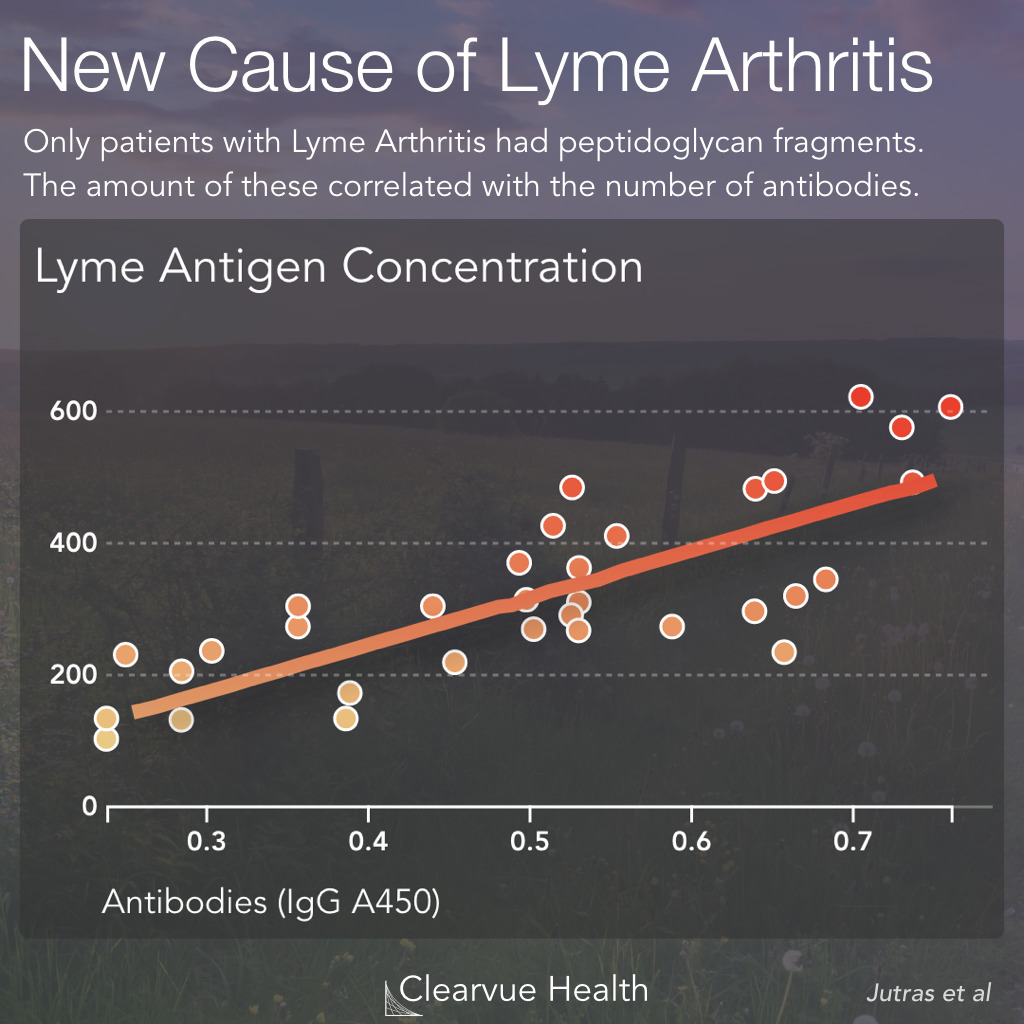
Figure 3: Lyme peptidoglycan in Lyme arthritis patients. Researchers found fragments of Lyme peptidoglycan in 32/34 patients with Lyme arthritis. The number of Lyme fragments correlated with the number of antibodies present to the fragment.
Researchers found this type of Lyme fragment in 32/34 Lyme Arthritis patients, including many who had received antibiotics, suggesting that this type of fragment may be common found in Lyme patients.
Additionally, they found evidence that Lyme arthritis patients with this type of fragment had developed an immune response to this fragment, which would cause the arthritis symptoms.
Antibodies are proteins created by your immune system. These proteins are used to recognize viruses, bacteria, and other particles that are foreign to your body. They are important for sensing invaders. However, they can also attack the body’s own proteins causing autoimmune disease.
How Common is Lyme Arthritis?

Figure 4: Lyme Arthritis Prevalence Data. Arthritis is relatively common in Lyme Disease. Around 60% of Lyme Disease patients will develop joint pain and swelling. Around 10% will have persistent symptoms after 6 months.
This is a relatively important finding because a significant portion of patients with Lyme Disease have lingering symptoms that are not treatable and often go unnoticed by doctors.
About 10% of patients with Lyme Disease report lingering arthritis and myalgia symptoms months after the original diagnosis.
Arthritis is a condition that refers to inflammation in joints. It most commonly refers to rheumatoid arthritis, which is an autoimmune disease, and osteoarthritis, which is caused by cartilage erosion.
Many doctors have not traditionally taken these complaints seriously since there has not been a known biological mechanism.
If this mechanism is supported by future studies, it would suggest that chronic Lyme Disease may actually be a real condition for many patients.
According to the authors, they also suggest that this condition maybe better treated with a different type of medication not often used today in Lyme patients.
Many patients with Chronic Lyme Disease today are treated with antibiotics, which may not work for this mechanism, as these "Lyme fragments" persist long after the Lyme bacteria themselves are killed.
Instead, the authors suggest that an anti-inflammatory treatment targeting the inflammation itself may work better:
“
The persistence of immunogenic PGBb material in inflamed joints provides a stronger rationale for targeting innate immune responses with medications, such as TNF or NF-κB inhibitors, for the treatment of such patients.
Centers for Disease Control
Why some patients experience PTLDS is not known. Some experts believe that Borrelia burgdorferi can trigger an “auto-immune” response causing symptoms that last well after the infection itself is gone. Auto–immune responses are known to occur following other infections, including campylobacter (Guillain-Barré syndrome), chlamydia (Reiter’s syndrome), and strep throat (rheumatic heart disease). Other experts hypothesize that PTLDS results from a persistent but difficult to detect infection. Finally, some believe that the symptoms of PTLDS are due to other causes unrelated to the patient’s Borrelia burgdorferi infection.
National Institutes of Health
These studies reinforced the evidence that patients reporting PTLDS symptoms have a severe impairment in overall physical health and quality of life. However, results showed no benefit from prolonged antibiotic therapy when compared with placebo in treating those symptoms.
IDSA
The prospective, controlled clinical trials for extended antibiotic treatment of Lyme disease have demonstrated considerable risk of harm, including potentially life-threatening adverse events...Prospective, controlled clinical trials have demonstrated little benefit from prolonged antibiotic therapy.
Clearvue Health is not affiliated with above organizations. The information above is provided to highlight and link to useful further reading.