Herd Immunity: How it Works
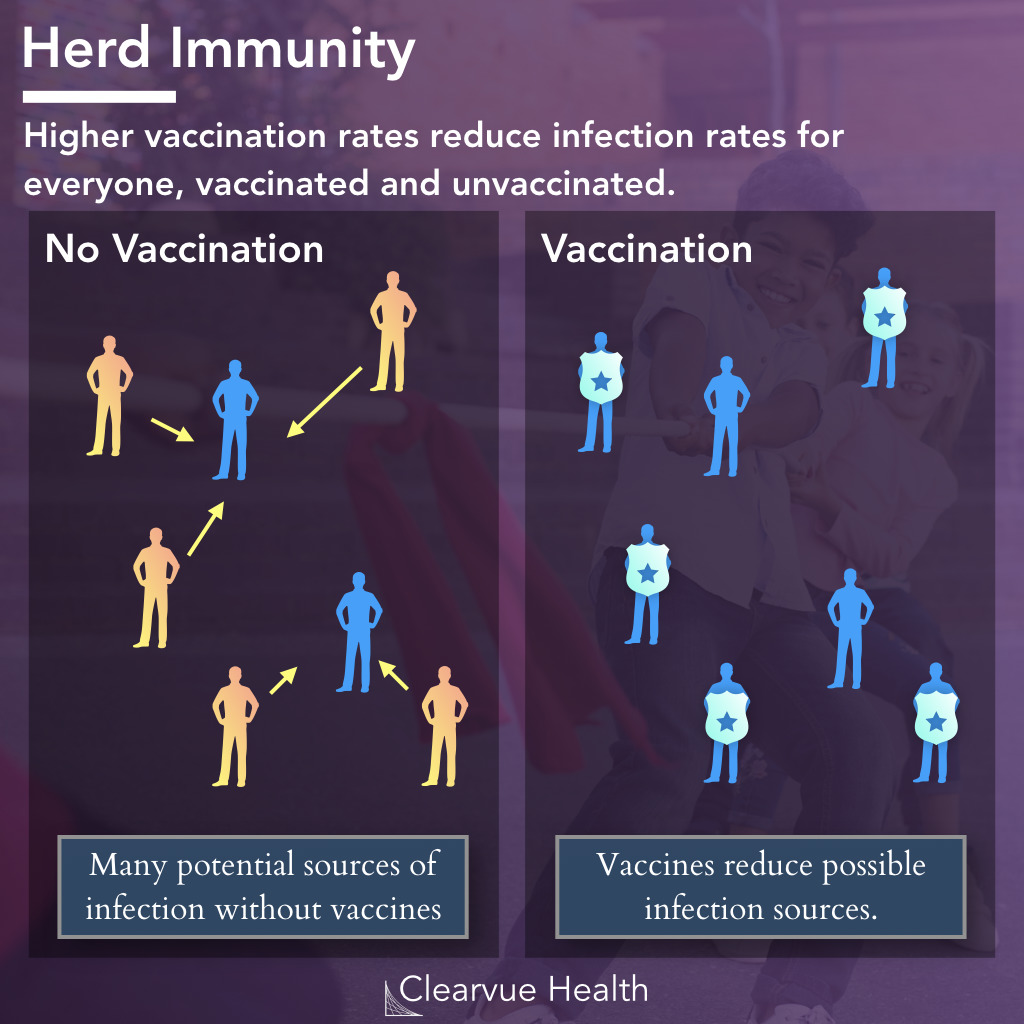
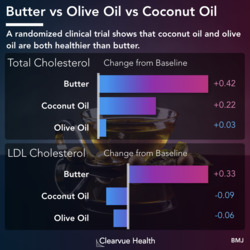
Figure 1: How Herd Immunity Works.
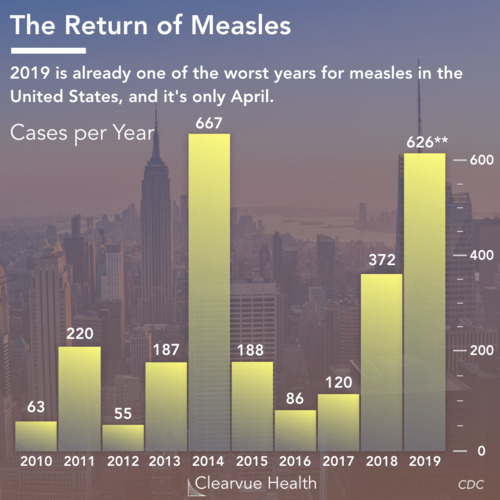
Herd immunity refers to the mechanism in which people who get vaccinated not only help themselves but their entire communities as well.
Within a community that is unvaccinated and vulnerable to a disease, any of your neighbors could become potential sources of an infection. Similarly, if you get an infection, you could pass it on to other neighbors or classmates or co-workers. This is how epidemics are formed.
In a community that has high vaccination rates, fewer individuals are available for a virus or bacteria to transmit itself to. Someone who gets sick, perhaps from travel abroad, would not be able to pass it on to neighbors. These vaccinated neighbors thus protect their entire community.
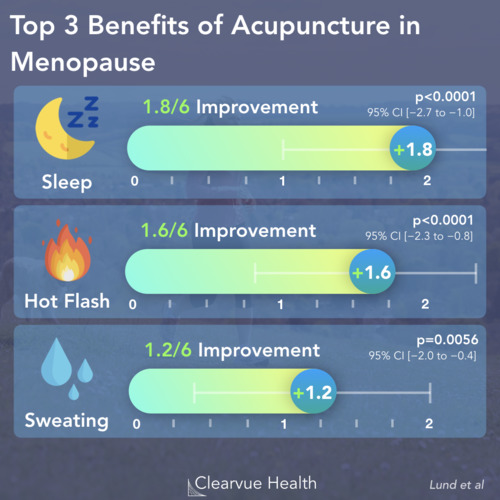
Effectiveness of the HPV Vaccine
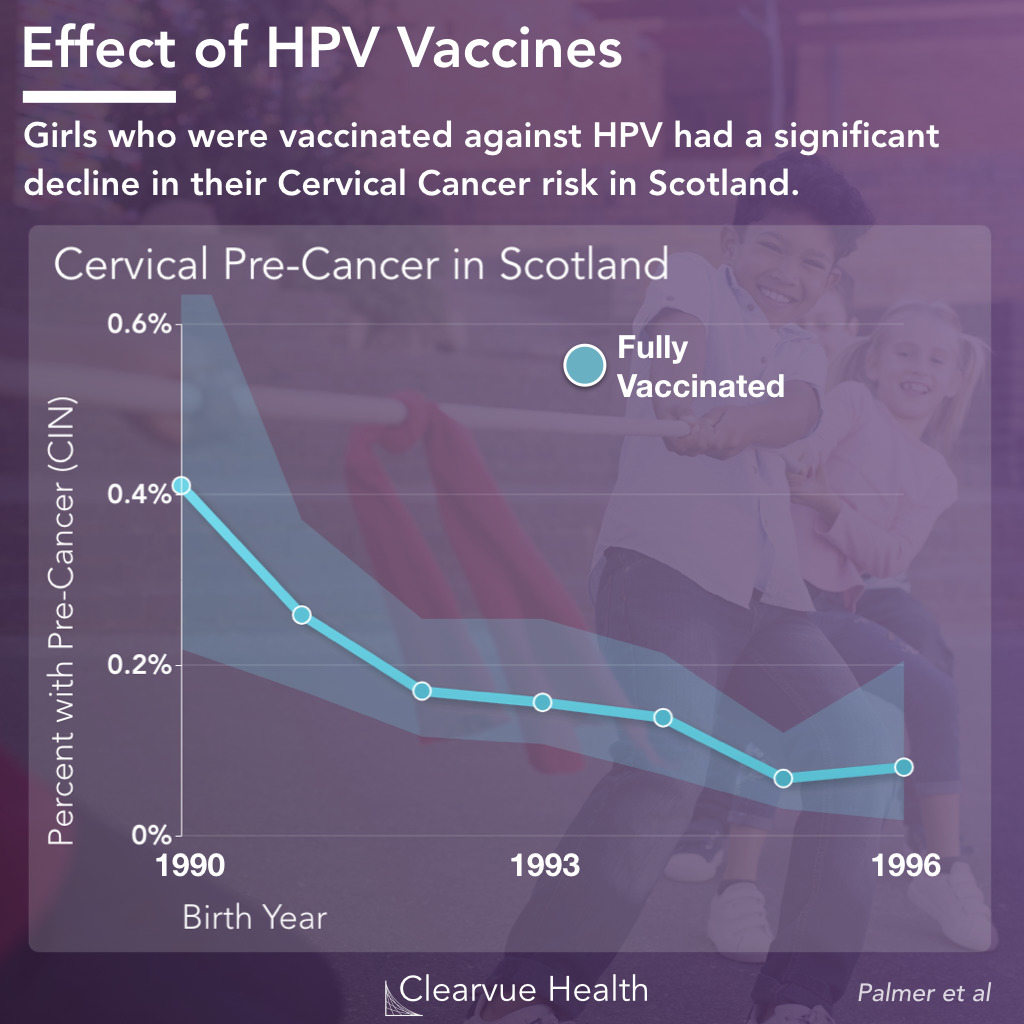
Figure 2: Effectiveness of the HPV Vaccine. Individuals who received the HPV vaccine had a dramatically reduced rate of cervical pre-cancer in Scotland. The line in blue represents the percent of patients with CIN Grade III or higher. The area around the line represents the confidence interval.
A new study out of Scotland provides a prime example of the herd immunity and the effectiveness of the HPV vaccine.
As expected, girls who received the HPV vaccine had a significantly lower risk of HPV, and this risk only decreased as more girls got vaccinated.
Source: Prevalence of cervical disease at age 20 after immunisation with bivalent HPV vaccine at age 12-13 in Scotland: retrospective population study
HPV Herd Immunity Statistics
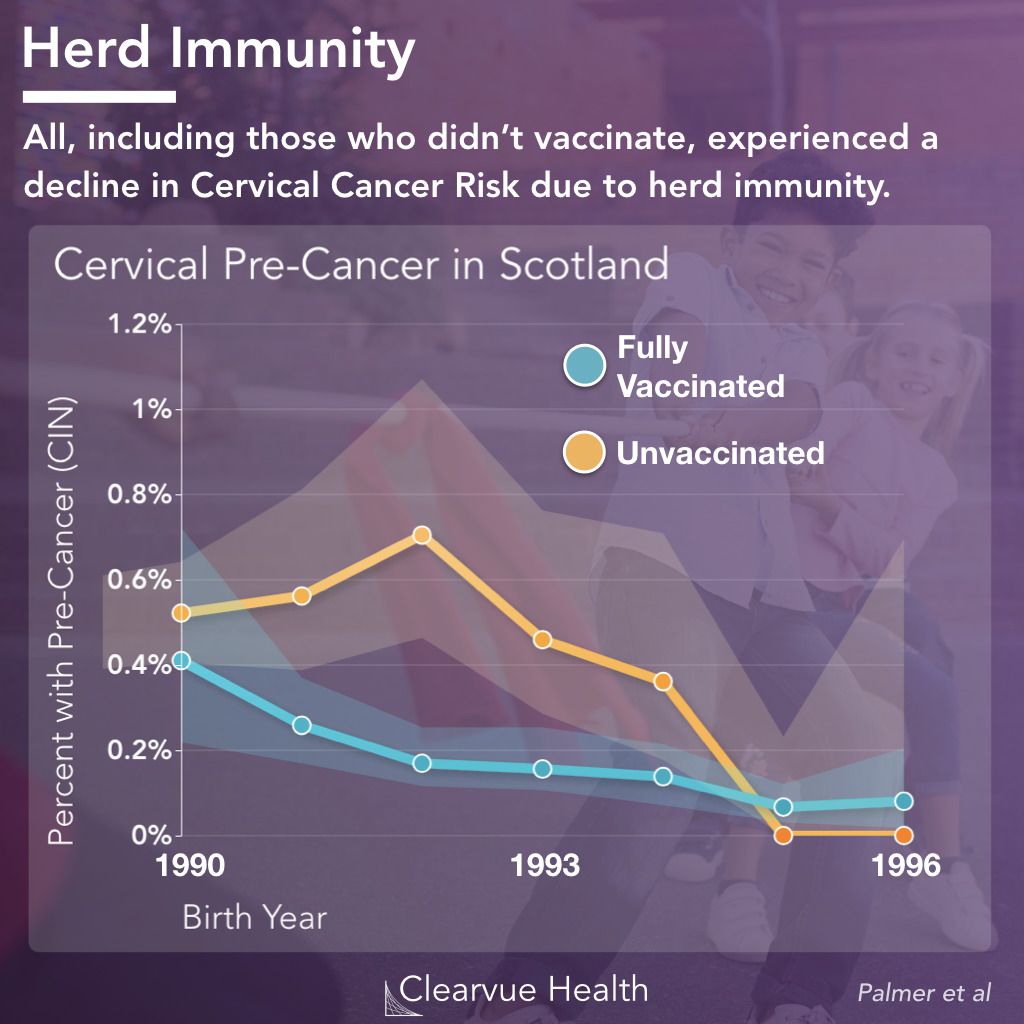
Figure 3: HPV Herd Immunity Statistics. The minority of girls who did not receive the HPV vaccine in Scotland also had a reduced rate of cervical pre-cancer. The lines represents the percent of patients with CIN Grade III or higher. The areas around the lines represents the confidence intervals.
While the majority of girls got vaccinated, not all girls received the HPV vaccine. Because of herd immunity, the girls who did not receive the HPV vaccine also benefited from lower cervical pre-cancer rates and reduced cervical cancer risk.
They were in essence protected by their neighbors who got vaccinated.
However, it is important to note that this does not remove the need for individual vaccinations. Not getting vaccinated makes you and your community for susceptible to infections:
“
For many diseases children, and in particular young children, are at the highest risk of the disease and also have the most severe illness. The best way to protect someone against a disease is to vaccinate them directly, rather than rely on ‘indirect’ protection through herd immunity. If someone who is unvaccinated does meet the germ responsible for that disease they will be completely susceptible.
Oxford Vaccine Group
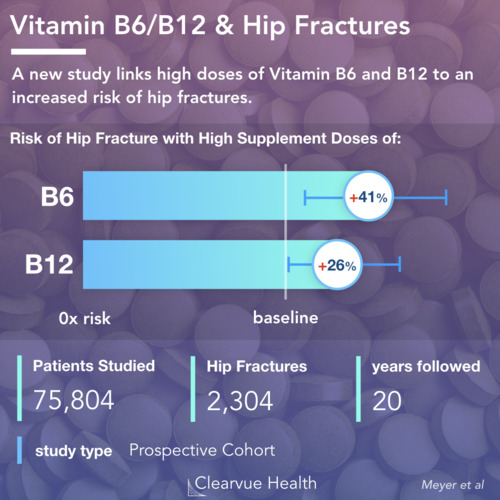
Cancer Risk and Vaccine Doses
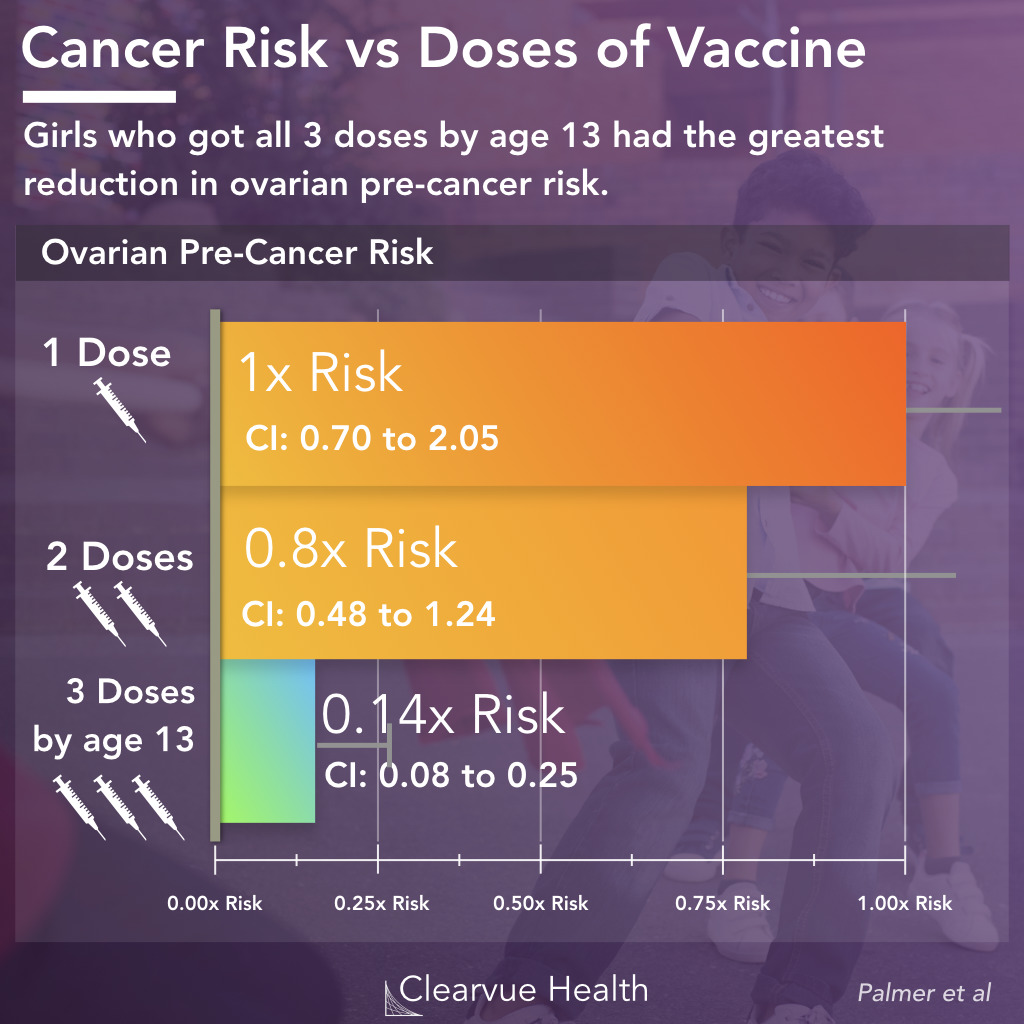
Figure 4: All 3 doses are required for full protection from HPV. Individuals who did not receive all 3 doses did not have a significantly lower risk of cervical cancer. The colored lines represent the odds ratios for CIN Grade III or higher. The bars represent the 95% confidence intervals of the odds rations.
The vaccine administered required multiple doses for full protection. Researchers found that only patients who received all 3 doses received the full benefits of HPV vaccination.
Patients who received one or two doses did not have a significantly lower risk of cervical cancer.
This suggests that if you are going to go through the pain and trouble getting the first dose of the vaccine, be sure to get all three. There’s not much partial protection offered by incomplete dosing.
Of note, the HPV vaccine is designed to reduce cervical cancer. Many cases of cervical cancer are caused by the HPV virus, which mutates genes critical to cancer protection. These data, along other studies, confirm the importance of HPV vaccination for cancer prevention. As the authors state:
“
These findings supplement previous studies in Scotland and the Netherlands, which indicate that the bivalent vaccine will afford protection against most HPV related cervical cancers.
Source: Prevalence of cervical disease at age 20 after immunisation with bivalent HPV vaccine at age 12-13 in Scotland: retrospective population study
Cancer Risk and Age of HPV Vaccination
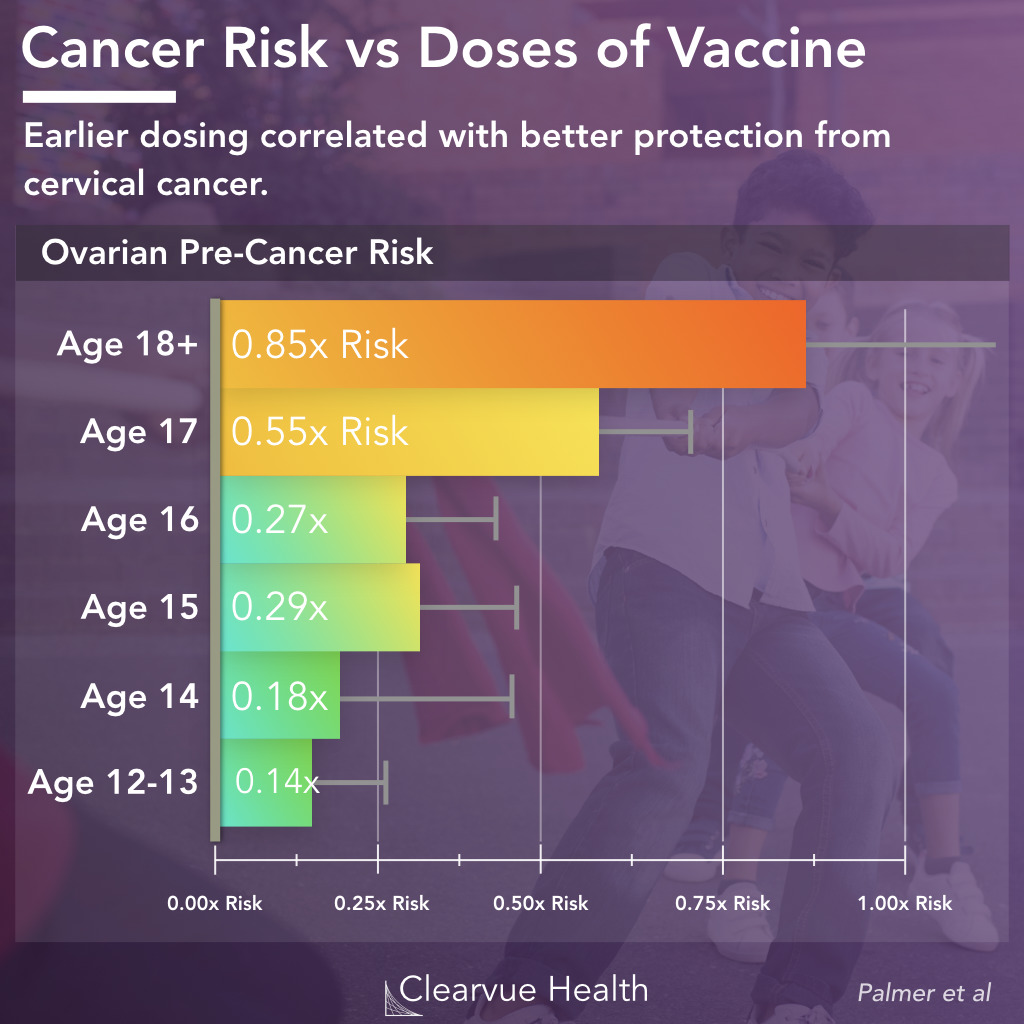
Figure 5: Cancer Risk and Age of HPV Vaccination. Getting the HPV vaccine as early as possible maximizes protection against cervical cancer. The colored lines represent the odds ratios for CIN Grade III or higher. The bars represent the 95% confidence intervals of the odds rations.
HPV vaccines work best when given prior to any exposure to HPV, which is known to increase with age. Getting it when it is too late offers less protection.
In this study, researchers found that girls who received the vaccine at age 12-16 had the highest reduction in cervical cancer risk. Meanwhile, girls who got vaccinated after age 18 did not show much protection.
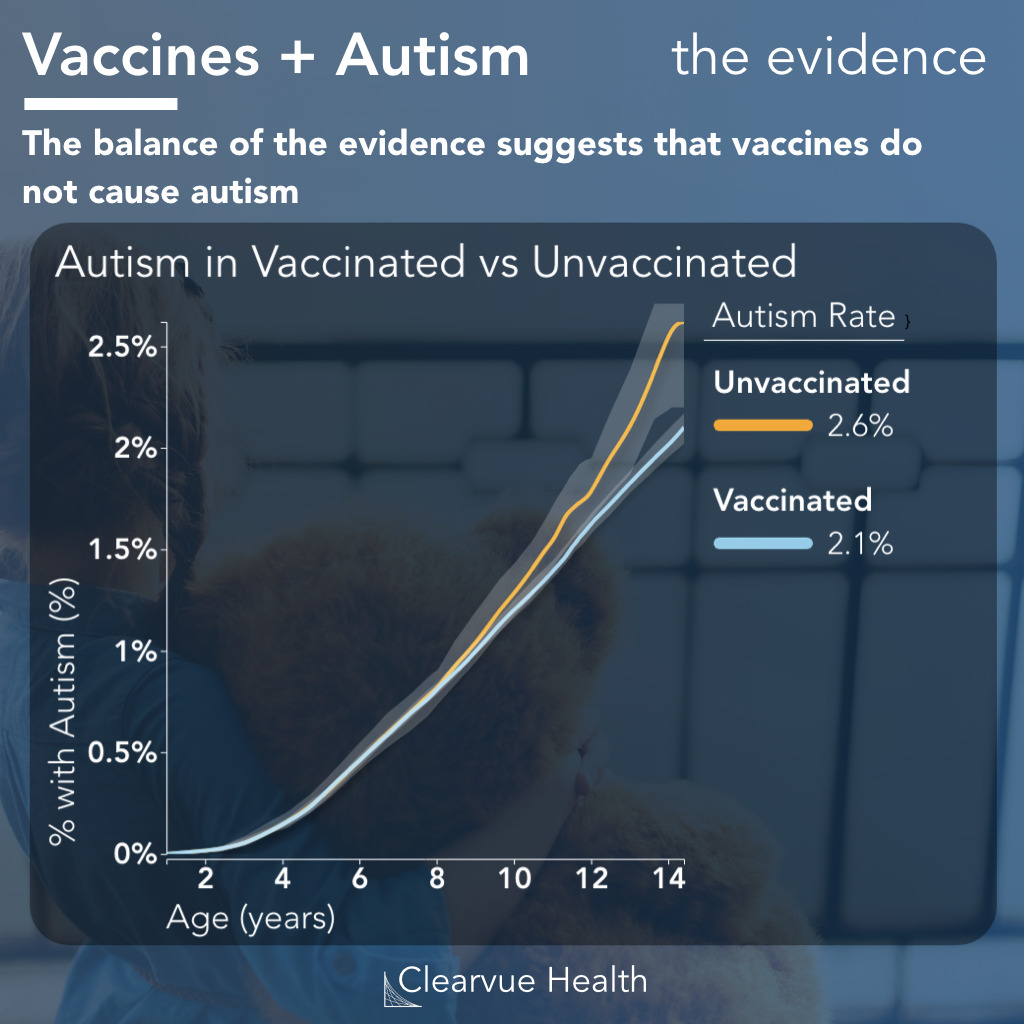
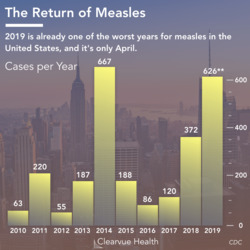
Related Article: Measles Vaccine
Another vaccine that is vitally important to children is the measles vaccine. In this article, we explore the data behind vaccines and autism.